![]()
Blog @ SunTech
Advice from the BP Measurement Experts
Blood Pressure Averaging in the SPRINT Study
In my last blog, I introduced some of the claims and confusion around the NIH Sprint study but today I’d like to clear up the main point of confusion and discuss the actual blood pressure (BP) reading technique used to obtain the SPRINT study’s “research readings”.
We will be examining the SPRINT claims of benefit to medicating to a Systolic BP of 120 mmHg, but that will be for another day. Today the focus is on BP averaging, how it was implemented in the SPRINT study, and why it makes sense even if you aren’t sold on the SPRINT findings.
Averaged BP readings are not new or limited to the SPRINT protocol. There are many benefits to taking an average BP over successive readings taken in succession while the patient sits in a calm state. There are papers dating back many years that show a correlation to ABPM study results [1] and a reduction in white coat hypertension [2][3]. So even if you are not sure about all the SPRINT findings, the techniques below could still prove valuable when diagnosing hypertension in your patients.
SPRINT BP Measurement Technique
A typical clinical BP measurement is a single reading taken with the clinician immediately present in the room during the entire measurement. Typically, in a clinical setting there is not a specified rest time before each reading. In contrast, the SPRINT measurements were largely performed using an automated BP spot check device with a programmed delay start. The delay allowed a specific rest time of 5 minutes followed by 3 readings at 1-minute intervals [4]. These readings were then averaged to obtain the single SPRINT study “reading”. The following infographic summarizes these differences.
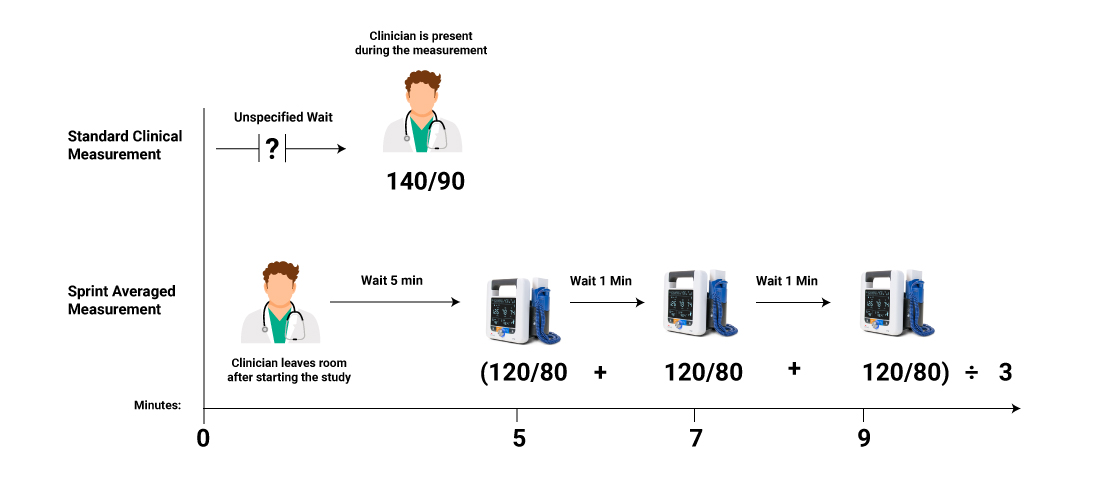
Clearly the SPRINT measurement technique requires significantly more elapsed time than a standard clinical measurement, however the majority of the time is unattended in the SPRINT study. At first glance, this seems to be in conflict with 80601-2-30 standards, which require the operator to be in attendance during the measurement and is further complicated by the fact that the SPRINT study appears to have been performed differently across its multiple test sites. [5] Interestingly, the 80601-2-30 standard does allow the patient to be the operator, but what does this mean in a clinical setting? Should the patient be instructed on what constitutes an unsafe condition and given instruction for removing the blood pressure cuff? Should they be given instruction to abort the reading? Or should they be trained on actual operation of the unit? We would like to hear from you, what do you think should be required to allow the patient to be the “operator”?
Equipment Considerations
If you might incorporate a BP averaging protocol in your practice, it is important that you consider a device that allows for a flexible averaging protocol while still offering a simple user interface. In my next blog we will consider the BPTru BP averaging protocol and how it differs from the SPRINT study. No matter what BP averaging approach you choose to take, the SunTech CT40 can easily be programmed to accommodate either protocol while also implementing a deceptively intuitive and simple user interface to minimize training requirements.
This is part 2 of 4 of a blog series on the Sprint Study. Stay tuned for the next blog articles.
References
- Godwin, Linda Beckett and Marshal. National Center of Biotechnology Information. BMC cardiovascular disorders. 5, 2005, Vol. 18.
- American Journal of Hypertension. Use of an automated blood pressure recording device, the BpTRU, to reduce the“white coat effect” in routine practice. [Online] June 1, 2003. [Cited: February 5, 2019.] https://academic.oup.com/ajh/article/16/6/494/128877.
- Circulation. 2016;134:904–905. DOI: 10.1161/CIRCULATIONAHA.116.022536. [Online] https://www.ahajournals.org/doi/pdf/10.1161/circulationaha.116.022536.
- Agarwal, Rajiv. Implications of Blood Pressure Measurement Technique for Implementation of [SPRINT]. Journal of American Heart Association. [Online] February 3, 2017. https://www.ahajournals.org/doi/abs/10.1161/jaha.116.004536.
- Huston, Larry. SPRINT: More Controversy And Confusion About ‘Landmark’ Trial. Cardio Brief. [Online] September 6, 2016. http://www.cardiobrief.org/2016/09/06/sprint-more-controversy-and-confusion-about-landmark-trial/.
- National Center for Biotechnology Information. The BpTRU automatic blood pressure monitor compared to 24 hour ambulatory blood pressure monitoring in the assessment of blood pressure in patients with hypertension. [Online] June 28, 2005. [Cited: February 5, 2019.] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1173098/.
Interested in getting more SunTech news, product info, as well as
tips, tricks, and insights from BP experts?
Sign up to get fresh content delivered direct to your inbox.