![]()
Blog @ SunTech
Advice from the BP Measurement Experts
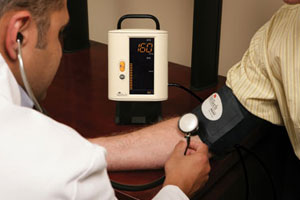
An Introduction to Automated Blood Pressure Monitoring
 Over the years, we’ve developed numerous white papers covering a wide range of topics. Through our work with hundreds of end users, we’ve discovered there are still elements of automated blood pressure monitoring that are misunderstood. As a result, we felt compelled to put together a comprehensive guide to automated BP monitoring to help increase knowledge and awareness. Much of this information has been pulled from our existing white papers that can be found at http://www.suntechmed.com/bp-devices-and-cuffs/suntech-247#White_Papers.
Over the years, we’ve developed numerous white papers covering a wide range of topics. Through our work with hundreds of end users, we’ve discovered there are still elements of automated blood pressure monitoring that are misunderstood. As a result, we felt compelled to put together a comprehensive guide to automated BP monitoring to help increase knowledge and awareness. Much of this information has been pulled from our existing white papers that can be found at http://www.suntechmed.com/bp-devices-and-cuffs/suntech-247#White_Papers.
First, we need to focus on why accurate blood pressure is important.
The New England Journal of Medicine published an interesting paper on blood pressure in its January 6, 2000 edition [1]. This study tracked the blood pressure measurements of 12,031 healthy men in six regions of the world for over 25 years. 1,291 of the subjects died from coronary heart disease (CHD). For an increase of 10 mmHg in systolic blood pressure, the relative risk of death from CHD rose by 28%. A 5 mmHg increase in diastolic blood pressure had a similar effect. These results closely match the outcomes of other ten-year studies from different regions of the world. They indicate the importance of small increases in blood pressure and the prerequisite of accurate blood pressure measurement.
This study underscores why an accurate blood pressure measurement is important. As we monitor our health, not having a true picture of blood pressure changes can result in a lack of treatment or proper management.
As we search for devices and techniques to improve patient care, some questions arise regarding the accuracy of automated devices. The most common being, “Why is my device giving me high readings?” Chances are, these automated readings are actually more representative of your true blood pressure because of the device’s built-in deflation rate and its clinically-validated and repeatable method of measurement.
As mentioned, automated monitors use an entirely different technique for blood pressure measurement.
Automated monitors measure BP differently than clinicians do. They employ a technique called “oscillometry,” which measures the pressure waves associated with the same sounds that clinicians listen for when they measure BP, called Korotkoff sounds; the latter technique is called “auscultation”. Oscillometry is used in a vast majority of automated BP devices because it has shown generally good agreement with auscultation [2]. However, there are times when the two techniques result in significantly different results. Thus, the BHS recommends occasionally checking the monitor against a mercury sphygmomanometer or other known pressure standard [3].
Above is the first major difference between traditional manual BP measurement and automated BP measurement. Another difference is the actual monitoring device. To ensure accurate BP measurement, a clinical-grade, validated device is most desirable.
Certification of medical devices in the United States is the responsibility of the Food and Drug Association (FDA). For blood pressure devices, the FDA relies upon the voluntary compliance by manufacturers to a standard developed by the Association for the Advancement of Medical Instruments (AAMI). However, lack of this designation does not prevent the sale of non-certified blood pressure instruments to hospitals, clinics, or individuals. Currently, no regulatory agency requires the use of AAMI-validated instruments. In fact, some of the most common automated blood pressure measuring devices have never passed AAMI certification [6]. Furthermore, the accuracy problems with inexpensive blood pressure devices such as those used for home monitoring are well-documented [7].
While it is critical to have an accurate device, many times there are ways to improve the accuracy of BP measurement through tried and true techniques. One of those is using a patient monitor that allows you to take both a manual reading and an automated reading which keeps more things constant (cuff, placement, deflation rate, etc.).
When in doubt, wait. This is frequently overlooked and can help your practice increase the accuracy of BP readings.
The American Heart Association (AHA) and the British Hypertension Society (BHS) recommend that clinicians allow a patient to sit still without talking for at least five minutes prior to measurement [2, 3]. For most patients, it is likely that the first measurement will be higher than the second regardless of the resting interval [4]
Having the correct size cuff is another critical factor for accurate measurements. Make sure that the correct cuff size is selected, and when in doubt, use a larger cuff.
In a study on cuff application, undercuffing accounted for 84% of cuff sizing errors [5]. These overestimations have been shown to be significantly larger than the errors using a cuff that is too large [2].
In the haste of improving patient throughput, a commonly overlooked factor is the cuff deflation rate. Many times, the deflation is performed much too quickly and can miss the Systolic measurement by 10-12 mmHg.
Deflating the cuff at 2-3 mmHg/sec, as recommended by the AHA and BHS, is the most difficult and important thing to do to ensure accuracy [2, 3].
Automated devices force a constant deflation rate, but if taking a manual reading, do not deflate the cuff more than 2-3 mmHg/sec. Odds are this will feel extremely slow…that’s because most readings are taken with a deflation rate much greater than the recommended rate.
So, how does one account for all of these complicating factors that are a part of measuring the two numbers that represent a patient’s cardiovascular health? While patience and understanding on the part of the clinician are required to ensure that BP measurements are carefully taken, different monitors or instruments are required as well. These devices should 1) employ clinical-grade automated technology, 2) allow clinicians to take a manual measurement with a stethoscope as do sphygmomanometers, and 3) encourage careful observer technique when taking measurements with a stethoscope.
1 van den Hoogen PC, Feskens EJ, Nagelkerke NJ, Menotti A, Nissinen A, Kromhout D. The relation between blood pressure and mortality due to coronary heart disease among men in different parts of the world.Seven Countries Study Research Group. New Engl J Med. 2000 Jan 6; 342(1):1-8.
2 Pickering TG, Hall JE, Appel LJ, Falkner BE, Graves J, Hill MN, Jones DW, Kurtz T, Sheps SG, Roccella EJ. Recommendations for Blood Pressure Measurement in Humans and Experimental Animals: Part 1: Blood Pressure Measurements in Humans: A Statement for Professionals From the Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research. Hypertension.2005; 45: 142-161.
3 British Hypertension Society. Blood Pressure Measurement With Mercury Blood Pressure Monitors. Poster: available from the British Hypertension Society at http://www.bhsoc.org/how_to_measure_blood_pressure.stm, accessed 6 Nov 2008.
4 Manning DM, Kuchirka C, Kaminski J. Miscuffing: inappropriate blood pressure cuff application. Circulation. 1983; 68(4): 763-766.
5 McAlister FA, Straus SE. Evidence based treatment of hypertension: Measurement of blood pressure: an evidence based review. British Medical Journal. 2001; 322: 908-911 (14 April).
6 Jones DW, Appel LJ, Sheps SG, Roccella EJ, Lenfant C. Measuring blood pressure accurately: new and persistent challenges. JAMA. 2003 Feb 26; 289(8): 1027-30.
7 James GD, Pickering TG, Yee LS, Harshfield GA, Riva S, Laragh JH. The reproducibility of average ambulatory, home, and clinic pressures. Hypertension. 1988 Jun; 11(6 Pt 1): 545-9.
Interested in getting more SunTech news, product info, as well as
tips, tricks, and insights from BP experts?
Sign up to get fresh content delivered direct to your inbox.



