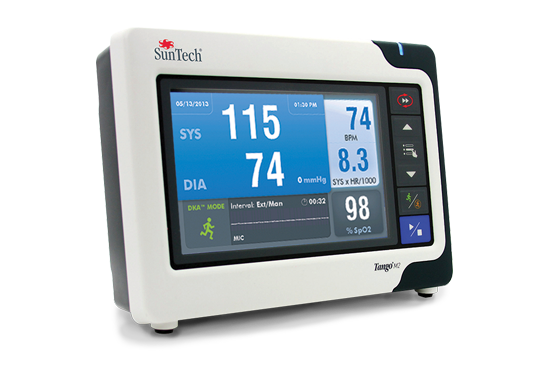
Tango M2 Stress Test Monitor
The Tango M2 Stress Test Monitor gives you the confidence to know that patient movement, mechanical vibration and observer variability won’t interfere with an accurate reading. Your focus can be where it matters most - on your patient.
Orbit-K Blood Pressure Cuff
We designed the Orbit-K Blood Pressure Cuff, specifically for cardiac stress and exercise testing applications. It enables repeated, reliable blood pressure measurements to be taken by maintaining proper placement for the length of the cardiac stress test - all while ensuring patient comfort is of the utmost priority. The Orbit-K Blood Pressure Cuff comes standard with our Tango M2 Stress Test Monitor and even has an added pocket to secure the microphone along the brachial artery.
Single Patient Use BP Cuffs for Tango M2
Infection control is a critical part of patient care. Having the right blood pressure cuff to support your efforts is extremely important, which is why we have created a line of Single Patient Use Blood Pressure Cuffs specifically for cardiac stress and exercise testing applications. These cuffs are made with a soft, yet durable fabric that ensures patient comfort and reliability.