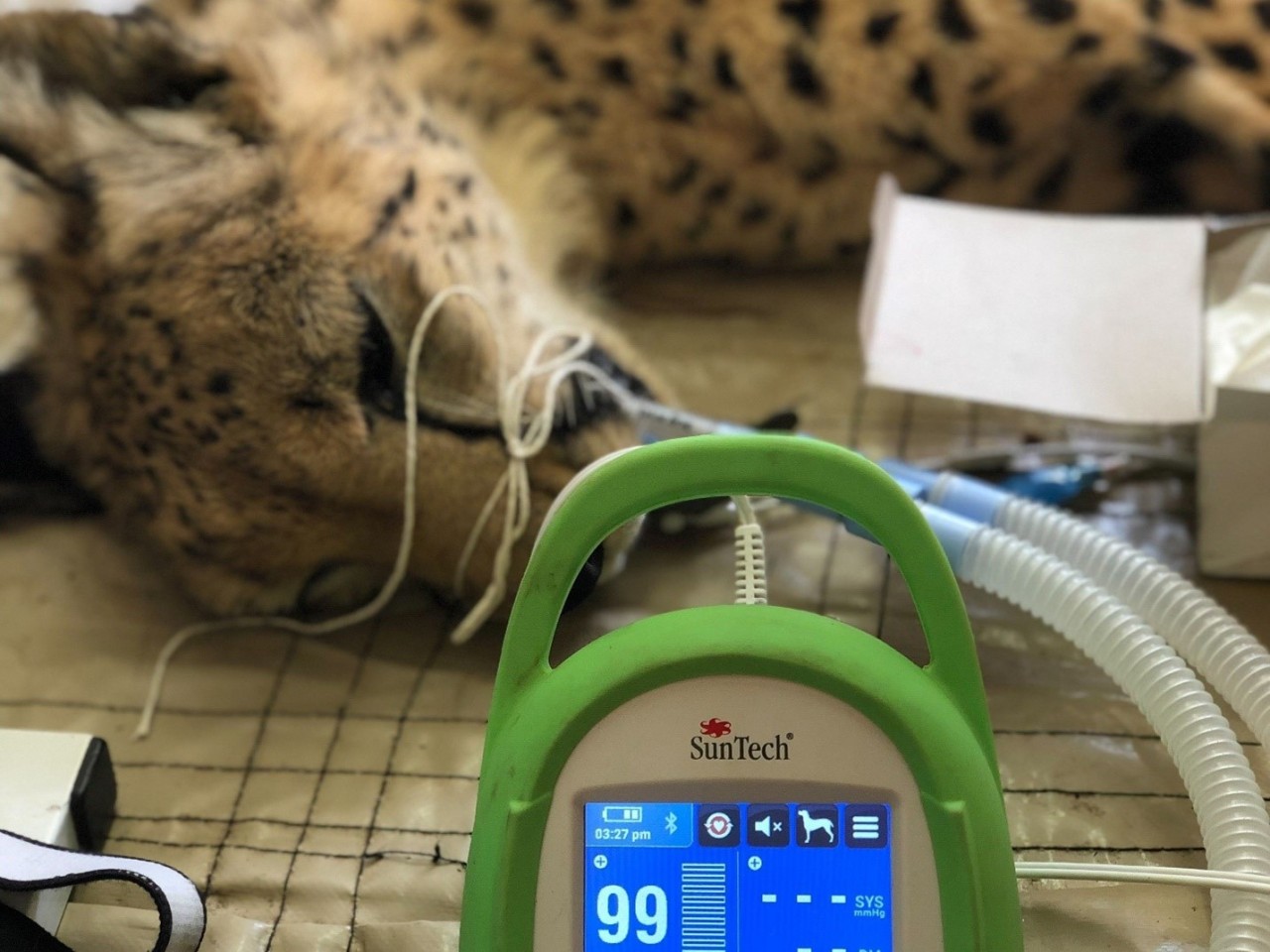
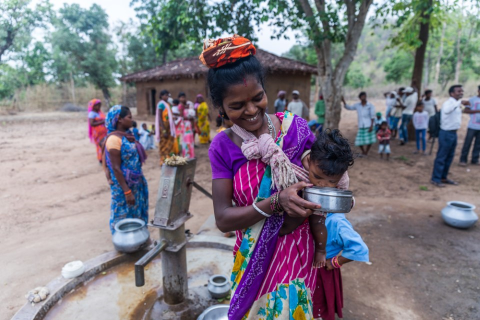We are excited to introduce the newest addition to the SunTech Vet BP lineup: the Vet40. The Vet40 is a surgical vital signs monitor designed for companion and equine patients. The Vet40 features SunTech’s proprietary animal-specific non-invasive blood pressure, temperature, pulse oximetry, electrocardiogram, and optional end-tidal CO2 and respiratory rate capabilities.
![]()
Blog @ SunTech
Advice from the BP Measurement Experts
By Dr Fabiola Quesada, DVM MsD MRCVS
Veterinarian
Co-Founder & Executive Director Wild Spirit Fund
CEO Wild Spirit
Background
Dr. Fabiola Quesada, DVM MsD MRCVS, is the Co-Founder & Executive Director at the Wild Spirit Fund. Wild Spirit Fund is a non-profit organization, born out of a decade of work in Africa and led by an international network of wildlife professionals, scientists, and veterinarians. Based in South Africa, their mission is to ensure the health and protection of wildlife in the natural ecosystem in which they live.
Wild Spirit Fund is based on the scientific movements of "Wildlife Conservation Medicine" and "One Health"; the former aims to identify the impact of the human footprint on the natural ecosystem; both assume the intimate correlation between the health of ecosystems, animals, and humans.
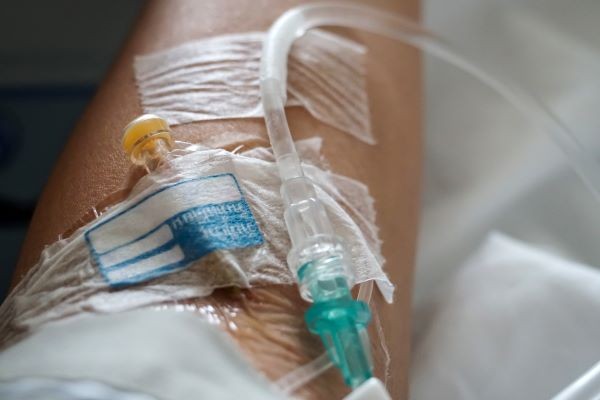
Medical device manufacturers are subject to many rigorous safety standards to ensure that patient’s lives are not endangered due to equipment related errors. One of these standards, ISO 80369-5, establishes a general framework and guidance for small-bore connectors intended for use in healthcare applications, promoting patient safety by reducing the risk of misconnections between different delivery systems.
ISO 80369-5 is a section of the ISO 80369 series of international standards titled “Small-bore connectors for liquids and gases in healthcare applications” which specifically applies to limb cuff applications. “Small-bore” refers to the size of the opening of the connector, in this case less than 8.5 mm. This article delves into the relevance of ISO 80369-5, its impact, and the steps medical device companies are taking to adhere to this standard.
The SunTech team would like to remind you about the importance of keeping a healthy heart 365 days of the year. Our 24hr ambulatory BP technology continually helps detect high blood pressure in a remote setting, allowing for patients to stay comfortable at home and for physicians to ensure test accuracy outside of a clinical setting.
In an effort to support widespread, life-saving initiatives, our SunTech family recently participated in the American Heart Association’s (AHA) Heart Walk. The heart walk is a 30-yr old, national event that serves as the AHA’s primary source for funding. Specifically, companies and individuals from around the country are encouraged to both participate in and fundraise for their local heart walk to help combat the No. 1 and No. 5 killers in our country: heart disease and stroke.
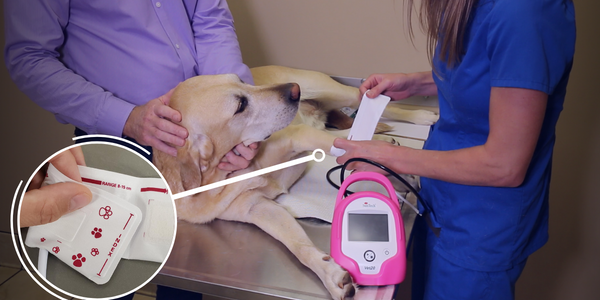
Cuff sizing should be easy, unlike the familiar and sometimes tedious process of wrangling a cat with a measuring tape. That is why at SunTech, we designed our vet cuffs with the users in mind. Our goal is to make your blood pressure measurements simple and effortless.
We understand that our monitors and cuffs are often used by busy veterinarians with patients of varying temperaments. So, to get rid of the hassle and to support accurate measurement techniques, SunTech veterinary cuffs are made with an index indicator and range markers to provide an efficient diagnostic experience.
Did you know that 1 in 4 people worldwide don’t have a safe, reliable water source? This heartbreaking statistic highlights the fundamental reason that the SunTech team, along with our parent company Halma and its subsidiaries, have been diligently working to raise resources and funds to help combat the global water crisis. As a part of these efforts, SunTech has held raffles, hosted silent auctions and conducted community-wide cleanup projects to aid us in achieving our goals. Our community is off to a strong start, having raised 78% of our $1,740 goal ($1,370) so far. This is a fantastic feat, and we believe that we can reach our goal with continued dedication and diligent awareness efforts. To donate, please visit our JustGiving page.
SunTech Medical recently released a new logo and overall brand refresh. Nothing about this change will impact the high level of service that we strive to provide each and every customer. However, we are sure there are questions about this rebrand and we wanted to help answer them. Please don’t hesitate to reach out if you have any other questions that aren’t answered here.
As patients, we expect our healthcare providers to consistently deliver accurate results that inform us on our health conditions. Yet, we often fail to hold ourselves to that same expected level of accuracy and control while we are caring for our own minds and bodies outside of a clinic.
Why then should accurate and controlled blood pressure monitoring be a priority?
As international leaders in the field of blood pressure diagnostics, we are familiar the difficulties and concerns related to controlling hypertension. Despite how hard controlling blood pressure can be, it is very important. Being equipped with the knowledge to control your BP can help empower you to take better control of your health. That’s why we, as well as the International Society of Hypertension, have gathered a list of helpful tips and tricks that you can adopt to help yourself decompress and control your blood pressure.
Eight simple suggestions for controlling your blood pressure: